Caregiving in northwest Syria
It is not sensible to compare the health system in areas outside the al-Assad regime’s control in Syria to its counterparts in Germany and Sweden or similar high-income countries. However, just discussing a health system, with what this term requires from the availability of a complex structure to the existence of clear and distinct components, is a kind of fantasy considering the current circumstances in northwest Syria. However, to be fair, we have to praise the efforts made to provide quality healthcare based on the application of the latest global recommendations, especially with regard to the rapid response to the Covid-19 pandemic in the these areas.
The NWS health sector was one of the most positively-affected sectors after the regime lost control of the area. It became more dynamic and flexible after being freed from the bureaucracy and corruption that restricted it under the Baath Party.
Below, I will try to shed light on a nascent experience reproducing one of the basic elements of health infrastructure in Europe – an element completely absent from health practice in Syria, despite the increasing need for it due to the war and large numbers of injured and disabled people fully dependent on the help and support of others.
We started by creating teams of students from the Faculty of Medicine at the University of Idlib to provide care and secure the basic needs of chronically ill and severely disabled people in the region. This was a completely new concept to the health culture in Syria. Reasons for this absence included limited financial resources, lack of trained staff, and socio-cultural (emotional) norms that oblige families of incapacitated patients to refuse outside help. Such help is perceived as a kind of insult and cause for shame. This mentality may even lead to accepting a patient’s miserable condition rather than accepting help. Therefore, the challenge was to transform this practice of professionalised care into a normal service that belongs to the community and can be accepted, to help break the stereotype that links it to the family institution abandoning its duties and solidarity with its members.
The idea originated from a group of Syrian diaspora doctors and started on a limited scale commensurate with the modest financing available and the strangeness of the idea to health and social identity in Syria. Medical students were chosen to ensure those involved had a medical background and provide them with much needed source of income for the costs of their studies. This job does not require medical experience, as nursing experience is needed to support those with chronic diseases and severe disabilities, but the medical training meant they were more readily accepted by families.
The coincidence of starting this group during the Covid-19 pandemic in northwest Syria made it more difficult in terms of the need for increased infection prevention measures to avoid transmitting the virus. Covid-19 infection prevention has proven exhausting for experienced teams, let alone a young team taking its first steps.
The current team, with modest resources, creates a file for each patient to include medical and pharmacological history and the type of help received. These data are discussed to identify any possible ways to improve quality of life for patients and delay the emergence of complications that may result from neglect or incorrect handling of their cases (e.g. diabetic feet, high blood pressure, arterial pressure, torsion ulcers).
Currently, nine community patients of different ages, five men and four women, benefit from this service. The youngest is thirteen years old, and the oldest is eighty. Of course, their needs vary depending on their injuries and the extent of their disabilities, but they share the need for regular care, continuous monitoring, and improved awareness of their needs and concerns.
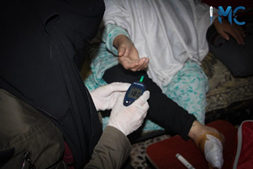
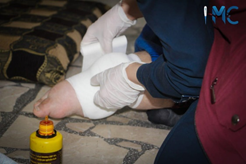
This service is provided through three daily visits in which medication is given, bandages are changed, immobile patients are turned over, and blood pressure and blood sugar measured if required. Patient hygiene and appearance are also taken care of, such as shaving if necessary. In the event of complications, consultations with specialized doctors are organised and participants transferred to hospitals when needed.
In parallel to the physical care provided, our team noted that most participants need psychological support, due to the poor care they suffered that deepened the psychological trauma caused by their disability. This was addressed by providing psychological support, which could be provided by specialist professionals in future, if resources allow.
The team started in March 2021 and the pilot is still new. It will need to be evaluated to measure the impact on the lives of participants and their families, and to try to develop it further. However, the urgency of the need for such a service is self-evident and it is important to draw the attention of charities and organizations operating in northwest Syria to this completely neglected area. This group of people is completely marginalized and deserves a better life than the current slow death sentence.
Mustafa Faham
Specialist in Internal Medicine, Bremerhaven Reinkenheide Hospital, Germany